Experimental drug could increase healthy fat levels
An experimental drug that boosts levels of healthy fats by modifying the expression of two newly described genes could have implications for the treatment of inflammation and diabetes.
In collaboration with a team from Lundbeck’s La Jolla-based research center, researchers from the Salk Institute and the Scripps Research Institute (all CA, USA) have discovered that an experimental drug can be used to boost levels of healthy fats – termed fatty acid esters of hydroxy fatty acids (FAHFAs) – in mice.
In 2014, the study’s lead author Alan Saghatelian (Salk Institute) and colleagues identified FAHFAs when they discovered a strain of diabetes-resistant obese mice. Further analyses revealed that the mice had FAHFAs at 16 times the base level.
The team went on to demonstrate that pre-diabetic individuals possess lower levels of FAHFAs in their blood and fat. Their findings suggested that increasing FAHFA levels could have a beneficial impact on human health. Further research has demonstrated that FAHFAs have anti-inflammatory effects and increase insulin sensitivity.
In 2016, Saghatelian’s group, in collaboration with Benjamin Cravatt’s team (Scripps Research Institute), identified AIG1 and ADTRP, two proteins that appeared to regulate FAHFA levels in isolated cells.
Now, both labs have teamed up with pharmaceutical company Lundbeck (Copenhagen, Denmark) to understand the mechanisms by which AIG1 and ADTRP regulate FAHFAs in animal models. It was discovered that in Aig1 and Adtrp double knockout mice, FAHFA levels were up to nine times higher in fat tissues when compared with their normal counterparts.
 Novel method could lead to non-invasive diabetes monitoring
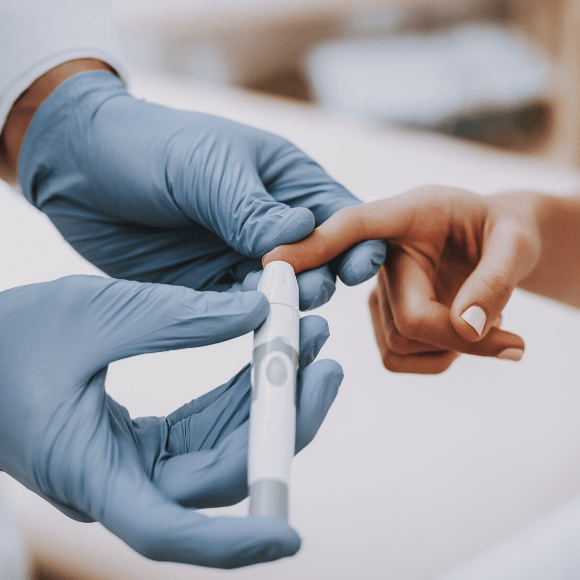
Novel method could lead to non-invasive diabetes monitoring
New research suggests that saliva could be utilized as a cheaper, pain-free alternative to blood for the monitoring of diabetes.
Additional experiments demonstrated that FAHFA levels were increased when Aig1 and Adtrp were repressed because the proteins no longer degraded them; however, levels of other fats were unaffected.
The team then identified ABD-110207, a small-molecule compound capable of blocking the action of both AIG1 and ADTRP.
“Until this point, we’d only ever studied the therapeutic potential of FAHFAs by feeding FAHFAs to mice,” explained first author Meriç Erikci Ertunc (Salk Institute). “That’s not a very natural situation, but we didn’t have any other way to alter levels until we generated mice lacking FAHFA degrading enzymes and found ABD-110207.”
Mice that were treated with ABD-110207 exhibited increased levels of FAHFAs, similar to those observed in the Aig1 and Adtrp double knockout mice. The metabolic benefits of consuming FAHFAs was not replicated in the knockout mice; the researchers attribute this to the different processing of ingested fats compared with those that the body naturally produces.
The team now plans to further examine the regulation of FAHFAs and their physiological function in the body. The findings could have implications for the understanding and potential treatment of inflammation and diabetes.