From sci-fi to reality: four futuristic advancements in biomaterials science

Biomaterials entwine the power of nature with human ingenuity – and they’re taking medicine by storm. Crucial to life science fields, including bioengineering and biotechnology, biomaterials can be natural or synthetic and are engineered to interact with living systems, often for medical purposes, such as to support, enhance or replace damaged tissue or biological function.
Their use dates back to antiquity, when ancient Egyptians used sutures made from animal sinew to facilitate wound healing. These days, as you might expect, biomaterials are significantly more sophisticated. Here, we explore some exciting preclinical advances in biomaterials science that may, with any luck, prove therapeutically beneficial, from a gel designed to heal chronic wounds to engineered ear cartilage and 3D-printed soft robots.
Novel biomaterial inspired by animal muscle
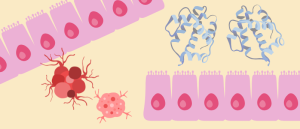
Engineers from Washington University in St. Louis (MO, USA) and Northwestern University (IL, USA) have created a novel biomaterial from genetically modified microbes that behaves just like animal muscle fibers. This protein-based material could transform medicine, textiles and agriculture.
Natural muscle fibers have intriguing mechanical properties, thanks to diverse protein domains that are largely unexplored for material design. For example, Immunoglobulin-like (Ig) domains act like molecular springs that can contract and stretch without losing function. They are therefore promising candidates for next-generation protein-based materials.
Seeking to harness this tensile strength and durability, the researchers took a synthetic biology approach, microbially synthesizing Ig domains.
The domains were created from several muscle proteins, including titin, filamin and myomesin, by engineering microbes in bioreactors. These were then processed into macroscopic fibers via wet-spinning, before comprehensive mechanical and structural characterization was performed.
The resulting fibers successfully mimicked the properties of Ig domains at the macroscale. In particular, fibers derived from the protein filamin exhibited a unique combination of high tensile strength, toughness, energy-damping capacity, shape recovery and mechanical stability under high humidity and heat conditions.
The fact that the fiber does not shrink much under high humidity sets it apart from existing protein-based materials, as do its stable production and higher yield.
The findings, the researchers conclude, establish microbially synthesized Ig domains as a new class of biomaterial that could be very valuable for use in biomedical implants and tissue scaffolds, as well as designing active wear and even creating meat substitutes.
How do muscles repair damage? Newly discovered metabolic ‘switch’ provides an answer
Unveiling a cellular mechanism by which muscle stem cells repair damage, researchers spark hope for remedying muscle loss caused by injury, aging and weight-loss medications.
Oxygen-delivering hydrogel for healing chronic wounds
A self-oxygenating gel could help heal injuries and prevent amputation, with the potential to expedite the development of functional living tissues or even organs, suggests research led by the University of California, Riverside (CA, USA).
Bioengineered tissues often suffer severe hypoxia, which impairs cell viability and function and limits their application in organ-scale engineering and regenerative medicine. There are existing methods to deliver oxygen to these tissues, but they often fall short of providing sustained oxygenation before neovascularization.
To prevent hypoxia, the team developed a smart self-oxygenating tissue platform that uses a biogel combined with electrodes for on-demand, localized oxygen generation. The hydrogel electrolyte incorporates a bio-ionic liquid into gelatin methacryloyl, creating an electroconductive scaffold that supports both electrolysis and cell growth.
When paired with a small battery, the gel becomes a tiny machine, splitting water molecules to generate a steady stream of oxygen.
In vitro studies revealed that the oxygen-generating capability of the platform maintained cell viability and promoted vascularization under hypoxic conditions. Meanwhile, diabetic wound healing studies using mouse models demonstrated that the technology significantly accelerated healing of both chronic and non-chronic wounds, increased collagen deposition and promoted angiogenesis with minimal immune response.
As well as a potential role in wound healing, the biomaterial represents a solution for controlled, prolonged oxygen delivery within bioengineered tissues.
“This project can be seen as a bridge to creating and sustaining larger organs for people in need of them,” study lead Iman Noshadi concluded.
‘Mystery’ protein helps with wound healing, while also waving cancer red flag
A cancer biomarker with surprising second job could inspire new chronic wound therapies.
3D-printed soft robots
A new 3D-printing method from Harvard University (MA, USA) for building soft robotic material could enable complex robots with potential surgical uses.
The design of soft robots made from biocompatible materials is of growing interest in industries from healthcare to manufacturing, with potential applications including shape morphing, actuation and wearable devices. However, designing and controlling soft robots for such purposes continues to be a challenge.
Attempting to make some headway in this area, researchers turned to 3D printing, developing a fabrication method for creating soft robotic materials with embedded pneumatics that exhibit programmable shape morphing behavior.
The approach uses rotational multimaterial 3D printing – in which two materials can be printed simultaneously using one nozzle – to create long filaments with hollow channels that, when filled with air, allow the device to bend in particular ways.
The outer shell of the filaments is comprised of polyurethane, and the inner channel is made of a polymer called a poloxamer. By precisely controlling the nozzle design, rotation rate, extrusion rate and print path, the team can control the orientation, shape and cross-sectional area of the channels.
Once the outer matrix was cured, the inner ink was removed, leaving behind embedded channels that can be pressurized to deform, allowing the soft devices to expand, contract and grasp.
Putting the technique into practice, the team printed a spiral flower pattern and a five-digit ‘hand’ complete with bendable ‘knuckles’.
By enabling researchers to build soft robotic matter in intricate shapes, the innovation could be used to create surgical robotics or assistive devices in future.
Pulling the heartstrings: building vascular networks in human cardiac tissue
Insights into a novel method to 3D print vascular networks embedded in human cardiac tissue.
A lab-grown ear
Scientists from ETH Zurich, the Cantonal Hospital of Lucerne and the Friedrich Miescher Institute (all Switzerland) have taken a step toward creating an ear in the lab using a patient’s living cellular material. Based on human ear cartilage cells, the team generated elastic cartilage with mechanical properties similar to those of natural tissue.
Microtia is a congenital condition characterized by malformation of the external ear. The current gold-standard treatment involves harvesting rib cartilage, which is invasive and associated with donor-site morbidity, impaired aesthetics and unnaturally stiff ears. Engineering functional elastic cartilage would provide a better treatment option, but it remains an unmet challenge in regenerative medicine.
In this latest advancement, researchers engineered primary human auricular chondrocytes to generate functional elastic cartilage with near-native tissue properties. First, they extracted and cultured cells from human small cartilage, before embedding them in a bioink and using a 3D printer to form ear-like structures. The ears were then placed in an incubator and allowed to mature, which promoted the formation of type II collagen, elastin and glycosaminoglycans, just like in native ear cartilage.
The grafts maintained their structural integrity and elasticity for 6 weeks in a subcutaneous rat model and “represent the closest replication of native human elastic cartilage achieved ex vivo to date,” the study authors write.
As such, they lay the foundation for clinically viable, functional auricular grafts that could bring hope to patients with microtia.
“Our current study provides a good guide to the current state of research,” summarized lead author Philipp Fisch (ETH Zurich). “It shows how close we already are to recreating the human ear – and what’s still missing.”