Whole-cell vaccines reimagined: a new method against recurrent UTI?
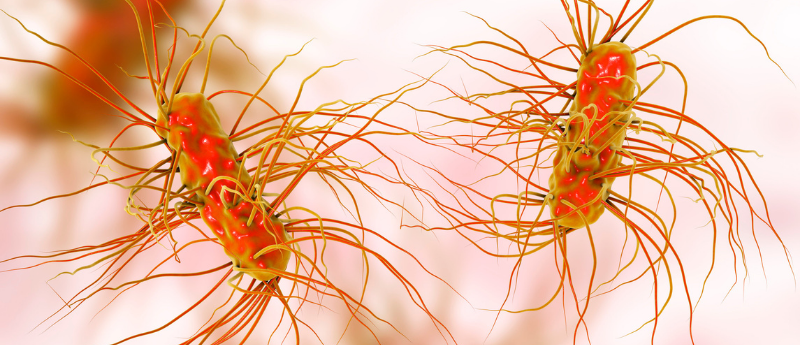
New encapsulating technology for whole-cell vaccines stimulates enhanced immunogenicity against Escherichia coli in a mouse model, shaping the future of urinary tract infection (UTI) vaccines.
Recurrent UTIs may soon be a thing of the past as researchers develop a new encapsulating technology for whole-cell vaccines. Co-senior authors Nicole De Nisco and Jeremiah Gassensmith (both University of Texas; TX, USA) collaborated on an interdisciplinary project developing a whole-cell vaccine for UTIs. The group demonstrated how their whole-cell bacteria encapsulated in a metal–organic framework (MOF) enhances antibody production in mice and provides a promising alternative to antibiotics and standard inactivated vaccines.
UTIs present a major strain on the healthcare system, particularly in the era of antibiotic resistance. The American Urological Association estimates that 150 million UTIs occur globally each year, accounting for $6 billion in medical expenditures. Recurrent UTIs pose a threat to the health of many, particularly in post-menopausal women, which unless successfully treated can result in sepsis.
“Every subsequent infection becomes more difficult to treat,” De Nisco explained. “Even if you clear the bacteria from the bladder, populations persist elsewhere and usually become resistant to the antibiotic used. When patients accumulate antibiotic resistances, they’re eventually going to run out of options.”
 Controlling cells and proteins with new nanocomputing agents
Controlling cells and proteins with new nanocomputing agents
Researchers are looking at the potential to develop a nanoscale programming language after controlling a protein within a cell using nanocomputing agent-based logic gates for the first time.
Whole-cell vaccines are preferrable over traditional single-antigen vaccines in potentially fatal infections such as UTIs due to the size difference between bacteria and viruses; the bacteria simply have too many antigens for scientists to choose from. Creating a whole-cell vaccine enables presentation of all the pathogen antigens to illicit a more effective immune response.
However, the whole-cell approach also has its flaws. ”Vaccines using whole-cell dead bacteria haven’t succeeded because the cells typically don’t last long enough in the body to produce long-term, durable immune responses,” Gassensmith detailed. Tackling this issue, Gassensmith’s team developed MOFs that encapsulate and immobilize individual bacteria in a crystalline polymeric matrix able to withstand high temperature, moisture and organic solvents. ”It allows an intact, dead pathogen to exist in tissue longer, as if it were an infection, in order to trigger a full-scale immune system response,” Gassensmith explained.
The study demonstrated that the MOF whole-cell vaccine was effective against uropathogenic E. coli, which cause approximately 80% of all community-acquired UTIs. “When we challenged these mice with a lethal injection of bacteria, after they were vaccinated, almost all of our animals survived, which is a much better performance than with traditional vaccine approaches,” Gassensmith said. “This result was repeated multiple times, and we’re quite impressed with how reliable it is.”
The authors hope to test the antigen depot against other bacterial infections such as endocarditis and tuberculosis. Ultimately, this technology has the potential to help millions of patients if it can be applied broadly to bacterial infections, De Nisco claimed.