Optogenetics could revolutionize diabetes treatment
Researchers have engineered pancreatic beta-cells that produce large amounts of insulin in response to light. They have been demonstrated to act as an effective diabetes treatment in mouse models.
According to the Centers for Disease Control and Prevention (GA, USA), over 30 million Americans are affected by diabetes. Current diabetes treatment methods involve manual regulation of blood glucose, which can often lead to long-term harmful effects.
Now, researchers from Tufts University (MA, USA) have demonstrated that pancreatic beta-cells that have been engineered to produce insulin in response to light exposure could be used as a novel diabetes treatment method, without the common side effects experienced with currently available treatments.
Current diabetes treatments involve either administering drugs that enhance insulin production or directly injecting insulin in order to manually regulate blood glucose levels. Both cases result in suboptimal blood glucose regulation, with frequently occurring spikes and dips in glucose levels.
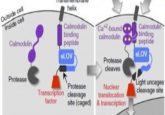
In the study, recently published in ACS Synthetic Biology, the researchers described their attempts to utilize optogenetics, a process where proteins change their activity in response to light, in order to develop a novel method for amplifying insulin production whilst maintaining the real-time link between insulin release and blood glucose concentration.
“There are several advantages to using light to control treatment,” explained Fan Zhang, first author of this study. “Obviously, the response is immediate; and despite the increased secretion of insulin, the amount of oxygen consumed by the cells does not change significantly.”
- Optogenetics: delivering deep brain genetic manipulation
- Could statins increase Type 2 diabetes risk?
- Downsizing diabetes
To achieve this, the researchers engineered pancreatic beta-cells, loaded with a gene that codes for a photoactivatable adenylate cyclase (PAC) enzyme. This method has previously been linked to increasing glucose-stimulated insulin secretion upon activation with light but had not been proven to improve diabetic state.
When exposed to blue light, the PAC produced cyclic adenosine monophosphate (cAMP) which increased insulin production in the beta-cell upwards of two-fold when blood glucose concentrations were high.
In the absence of glucose, there was no increase in insulin production. This is important as one of the common side effects of current diabetes treatment is the overcompensation of insulin, which can result in hypoglycemia.
Transplantation of these engineered pancreatic cells under the skin of diabetic mice resulted in improved glucose tolerance, lower hyperglycemia and higher levels of plasma insulin when exposed to blue light.
“It’s a backwards analogy, but we are actually using light to turn on and off a biological switch,” remarked Emmanuel Tzanakakis, corresponding author for this study. “In this way, we can help in a diabetic context to better control and maintain appropriate levels of glucose without pharmacological intervention. The cells do the work of insulin production naturally and the regulatory circuits within them work the same; we just boost the amount of cAMP transiently in beta cells to get them to make more insulin only when it’s needed.”
The results of this study present a novel solution to the issues seen in the current methods for diabetes treatment. The researchers intend to further develop the method, potentially by improving illumination and coupling to a glucose sensor in order to create a bioartificial pancreas device.