Novel drug combination converts glia to restore neuron function
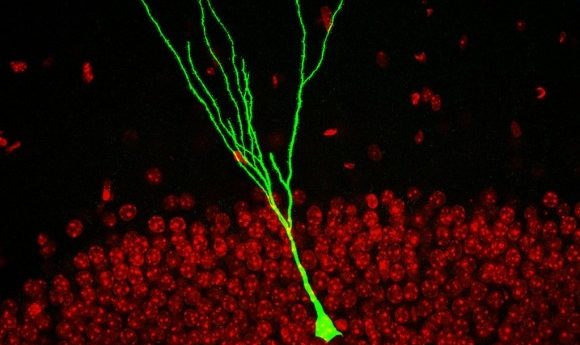
A new drug combination shows potential for brain repair by transforming glial cells into healthy, viable neurons, restoring neuron function. A new four drug combination therapy has been developed that could help restore neuron function by converting existing glial cells, adjacent to damaged or dead neurons, into healthy new neurons. The research behind the discovery was led by Gong Chen (Penn State University; PA, USA) and could prove pivotal in the treatment of an assortment of neurodegenerative disorders. The research team set out to address one of the key stumbling blocks in the treatment of neurodegenerative disorders. As Chen explains:...
To view this content, please register now for access
Join our member community for FREE to access a collection of journal and online-only features, including:
- Exclusive access to educational videos, eBooks and insights into top BioTechniques journal articles
- The latest news and journal updates delivered straight to your inbox when you want it
- Personalized recommendations for the latest member-exclusive podcasts, interviews and expert opinions
- Priority registration to webinars, panel discussions and events
- Access to competitions and journal publication discounts, including 10% off open access fees when you sign up today!